perianal fistual in GSD
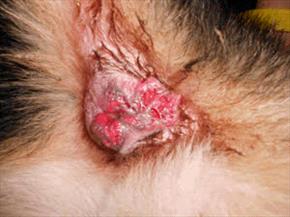
Perianal fistulas in a German Shepherd. Photo by MarVistaVet
(Also called perineal fistulae, anorectal abscesses, perianal fissures, perianal sinuses, and pararectal fistulae.)
Most people are not in the habit of inspecting the area under their dog’s tail unless the dog seems to be doing something that indicates a problem. Signs of a problem might include licking under the tail, scooting the rear end on the ground, or seeming to be in pain when sitting or raising the tail. When the tail is lifted and the anus inspected, a dog with perianal fistulae will show deep open crevices and some oozing pus all around the anal sphincter. It may not be possible to get a good look as pain may preclude lifting the tail, but odor may be noted, and the dog might be straining to defecate. There is also an association of perianal fistulae with the mucous diarrhea of colitis, so that might be seen as well. Perianal fistulae wax and wane but ultimately, over time, the condition is progressive, ulcerating the surface of the anus and its surroundings.
What Causes this Condition?
At this time, no one knows, but recent information suggests an immune-mediated basis. There also seems to be a genetic contribution as the German shepherd seems predisposed to the development of this condition; however, this phenomenon may be more about conformation than about a specific genetic factor for the disease.
While any breed can be affected, 85% of affected dogs are German Shepherd dogs. The anal glands may or may not be involved in the fistulation, but there seems to be a clear association with concurrent colitis (inflammation of the colon, as mentioned). Relative to other breeds, the German shepherd dog has an increased number of apocrine sweat glands, the type of sweat glands that produce unpleasant-smelling, oily sweat (as opposed to watery sweat) in the anal area. The average age of onset is five years, and approximately twice as many males are affected as females.
Approximately 85% of affected dogs are German Shepherd dogs.

Photo by Mary Buck
What Else Could It Be?
Several conditions can produce ulcerative lesions around the anal sphincter. While perianal fistulae have a typical history and appearance, it is important to get the right diagnosis. Some conditions that might look similar include:
- Squamous cell carcinoma of the anus (cancer)
- Hyperplastic anus (common in older unneutered male dogs)
- Perianal adenoma (benign tumor also common in older unneutered male dogs)
- Anal sac rupture
- Anal sac tumor
- Mucocutaneous lupus
Treatment
This condition is an immune-mediated disease. Treatment centers on suppressing the immune reaction that is causing the problem, and this means immunosuppressive drugs will be the centerpiece of therapy. Realize from the beginning that, while improvement is evident within a couple of weeks, it will take two to five months to get the lesions fully under control and that maintenance therapy may be needed for the remainder of the animal’s life. The good news is that control can usually be achieved and continued with maintenance levels of medication.
Immune Suppression
Years ago, an assortment of surgical procedures were used to trim the diseased tissues of the perineal fistulae, but immunomodulating drugs have largely supplanted surgery. In particular, two medications have emerged: cyclosporine (an oral drug) and tacrolimus (a topical drug). Many dogs will need both to control their disease at least at first, but often, the topical product can be used alone once the pain has been controlled.
Cyclosporine
Cyclosporine was originally developed for organ transplant patients to prevent organ rejection by modulating the immune response without necessarily suppressing it. The medication is given twice daily, and improvement should be seen within the first two weeks of use. Cyclosporine is an expensive medication, and there is tremendous controversy over whether or not generics are bioequivalent. Only microemulsion forms of cyclosporine are effective, which usually means a brand-name veterinary product. Higher-dose protocols seem to yield faster, more sustained results.
As mentioned, improvement is typically obvious within the first two weeks, though several months are needed to resolve lesions. After the disease is controlled, cyclosporine may be tapered off over another three to five months. Approximately 50% of dogs will not be able to fully discontinue medications, and their symptoms will recur within two to 12 months if a maintenance schedule is not implemented. This could involve tacrolimus (see below), cyclosporine, or both.
cured perianal fistulas
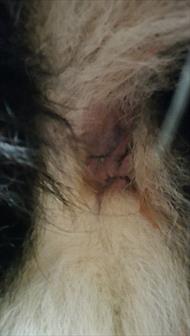
Same anal area as shown above after several months of cyclosporine therapy. Photo by MarVistaVet
Cyclosporine tissue levels can be boosted (and overall financial expense reduced) with the concurrent use of ketoconazole, an antifungal drug.
This trick can be used to cut the dose of cyclosporine and save money. There is controversy regarding whether blood levels of cyclosporine help determine the dose and what the relationship is between tissue levels and blood levels. Because of the long-term use needed to control perianal fistulae, it is best to monitor liver enzymes or liver function tests in the patient; cyclosporine blood levels may or may not be recommended by your doctor.
Tacrolimus
Tacrolimus is a much stronger immunomodulator than cyclosporine. Because it can be applied directly to the fistulae, high tissue levels can be achieved right in the area where they are needed. The potential for side effects and expense is also much more favorable than that of cyclosporine, but only 50 percent of dogs experienced resolution with tacrolimus alone after 16 weeks versus 85 percent with cyclosporine. In a perfect world, both oral cyclosporine and topical tacrolimus are used at the same time, but after the condition is controlled, tacrolimus alone can be used to prevent recurrence. It is important to wear gloves when applying tacrolimus as this medication has been linked to an increased risk of cancer in humans but not in dogs.
Other Options
Cyclosporine currently dominates treatment for this condition, but it is an expensive drug, and it may not be feasible to use it for months on end in a large-breed dog. In this event, prednisolone has been used, but there are undesirable side effects with high-dose steroid use (extreme thirst, increased appetite, weight gain, panting, muscle loss), and approximately 30 percent of dogs will not respond.
Azathioprine is a stronger immunosuppressive drug. The above side effects are not associated with its use, though bone marrow suppression is possible, and some monitoring tests are generally recommended. Because it takes some time to exert its effects, it is commonly combined with prednisolone, at least at first.
Approximately 50 percent of dogs were able to achieve remission with azathioprine in combination with a limited-ingredient diet (see below).
Supportive Therapy Beyond Immune Suppression
Antibiotics
Since these lesions are commonly infected, at least at the beginning of treatment, antibiotics are typically prescribed. A topical antibiotic may be helpful for long-term infection control. However, it is important to realize that antibiotics alone will not control this deeply rooted problem; they are merely adjunctive to controlling complicating infections.
Stool Softeners
Because of the ulcerations, defecation may be painful. To minimize the straining, stool softeners may be prescribed.
Novel Protein / Limited Ingredient Diet
Food allergy seems to be a possible etiology in this condition, so using foods that the patient could not possibly be allergic to has been recommended as an adjunctive therapy. Such diets are typically made from unusual protein sources such as rabbit, duck, kangaroo, fish, or venison. Most veterinary hospitals stock appropriate food. It is important to note that there is nothing especially hypoallergenic about these unusual proteins; the idea is that the patient has likely never eaten them before. If the patient has never been exposed to these proteins, there should be no possibility of allergy, as developing an allergy requires multiple exposures to a protein. In one study, 50 percent of the dogs with perianal fistulae also had colitis (colon inflammation and associated mucous diarrhea). If this is not a coincidence, then the fistulae should respond to some of the treatments that help colitis, and this would include a hypoallergenic diet.
Surgery: If Immune Suppression Fails
Before we had cyclosporine, perianal fistulae were treated surgically with mixed results. Presently, surgery is only recommended for patients for whom immunosuppression has failed or where the anal glands are involved. The goal of surgery is to remove the proliferative or dead tissue, prevent or treat any anal or rectal strictures (narrowed areas caused by scarring), and change the “environment” of the perineal region. Tail amputation may be required; in one study, tail amputation alone was 80 percent successful in preventing recurrence.
If the anal glands are involved in the fistulae, they will have to be removed. In milder cases, chemical cauterization of fistulae (which destroys abnormal tissue and allows normal tissue to heal) may be helpful. Cryotherapy, where a freezing agent is used instead of a chemical one, has been less effective (more scarring, less control over the area treated, etc.) Laser therapy, on the other hand, has been 95 percent successful in preventing recurrence and controlling pain (20 percent of patients developed fecal incontinence, but most of these cases were controlled with diet).
The more extensive the surgery, the greater the potential for complications. Stool softeners are typically needed for a month after surgery, and the owner should be comfortable cleaning the anal area. Fecal incontinence, a narrowed anus, and inability to control the fistulation are the chief complications with surgery.