(Immune Destruction of Blood Platelets, also called ITP or IMT )
What is a Platelet?
Formed elements of blood
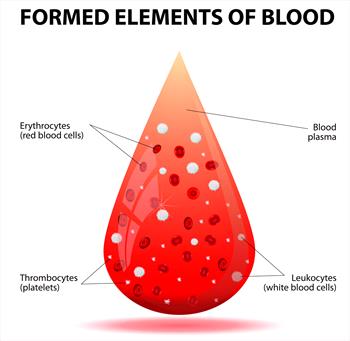
A platelet is a cloud-shaped blood cell, neither related to the red blood cell line nor the white blood cell line. Platelets assist in the clotting of blood in that they home in on damaged areas of blood vessels and aggregate there, meaning that they pile onto each other and bind, forming a small plug to seal the hole in the leaking blood vessel. While piled on each other, they release assorted biochemicals that initiate a more permanent fibrous seal of the tear. Of course, large tears are too big for platelets to seal but when it comes to small bleeds and normal blood vessel wear and tear, platelets are the star of the show.
There is a saying that “platelets are vascular integrity and vascular integrity is platelets.”
A small bleed unstaunched by a platelet aggregation quickly becomes a large bruise. Spontaneous bruising (in other words, visible bruising from the normal wear and tear of one's body) is a sign of reduced platelet numbers or poor platelet function.
Small abnormal bruises are called petechiae or petechial hemorrhages. Large abnormal bruises are called ecchymoses or ecchymotic hemorrhages.
Platelets in Times of Health
Platelets come from the bone marrow, where very large cells called “megakaryocytes” spit off little active pieces of themselves.
At any given time, some 200,000-500,000 platelets are on patrol in the circulation, though only about 20,000 to 50,000 are considered the bare minimum to prevent spontaneous bruising and bleeding. About 1/3 of the circulating platelets are actually stored in the spleen, like boats in a harbor, ready to mobilize if necessary. The rest are "on duty."
When platelets become too old to be useful or the immune system marks them as damaged, the spleen and liver have special cells which essentially eat old blood cells (not just platelets) and recycle their inner materials. New cells come out to replace them, and there is a balance between the release of platelets and the removal of platelets.
This is reviewed because the excess removal of platelets creates a platelet deficiency, which is concerning.
These pieces are platelets, ready to enter circulation, where they will live for an average of 8 to 12 days in a dog or 6 to 8 days in a human before a bleeding capillary calls them to their destiny. At any given time some 200,000 to 500,000 platelets are on patrol in the circulatory system, though only about 20,000 to 50,000 are considered the bare minimum to prevent spontaneous bruising and bleeding. About one-third of the circulating platelets are stored in the spleen, like boats in a harbor, ready to mobilize if necessary. When platelets become too old to be useful, the spleen has cells called phagocytes that essentially eat old cells and recycle their inner materials.
Immune-Mediated Platelet Destruction
There are many reasons why platelets can be marked for removal. When this happens, antibodies coat the platelets and the spleen's removal system takes them out of circulation. If the immune reaction is amped up, platelets can be removed at up to ten times the normal rate, overwhelming the body's ability to replace them.
If the marrow successfully receives the message to make more platelets, the megakaryocytes there respond by getting larger and growing in numbers so that they may step up production. The platelets produced under these circumstances tend to be larger and more effective than normal platelets and are called "stress platelets." Unfortunately, they die off after a day or two instead of the usual 8-12 day platelet lifespan. If antibody levels are high, a platelet may survive only minutes or hours after its release from the bone marrow.
Making matters worse, antibody-coated platelets that are still circulating do not function normally. This is balanced by the especially effective stress platelets entering the scene so that overall it is hard to predict how the balance will work out in a given patient.
Why Would the Immune System Attack the Body's Own Platelets?
Keep in mind that the immune system responds to the shapes of proteins present on a cell’s surface. These shapes are similar to ID cards. The immune system recognizes shapes defined as “self” and does not attack but when it sees a cell expressing protein shapes that are “non-self,” it will respond.
If the immune system is responding to a blood parasite, tumor, drug, or other cell type (as in lupus or immune-mediated hemolytic anemia), it will be producing antibodies against enemy shapes. Some of these shapes may, unfortunately, resemble some “self” shapes such as some of the shapes on the surface of the platelets. The platelets are then misidentified as the enemy and are attacked.
What Happens to the Patient?
The usual patient is a middle-aged dog. Poodles appear to be predisposed, although Cocker Spaniels and Old English Sheepdogs also seem to have a higher than average incidence of this condition.
Spontaneous bruising is the major clinical sign. The gums and oral surfaces, as well as the whites of the eyes, are obvious areas to check, as is the hairless area of the belly. Small spots of bruising in large conglomerations called petechiae (pet-TEEK-ee-a) are the hallmark sign. A large, purple expansive bruise might also be seen, which is called ecchymosis. Large internal bleeds are not typical of platelet dysfunction, though bleeding small amounts in urine, from the nose, or rectally may also indicate a platelet problem.
When these sorts of signs are seen, a platelet count is drawn, along with usually an array of clotting parameters, red blood cell counts to assess blood loss, and other general metabolic blood tests. Since reliable testing to detect anti-platelet antibodies is not available, the veterinarian must determine if any other possible causes of low platelet count make sense.
Causes of Platelet Reduction
Dramatic reduction in platelet numbers is almost always caused by primary immune-mediated destruction, which means there is no apparent cause; the immune system just went haywire. That said, it may be worth making an effort to identify a blood parasite or other cause of the platelet drop.
- Ehrlichiosis (especially infection with Ehrlichia platys, which has recently been renamed Anaplasma platys)
- Rocky Mountain Spotted Fever (Neorickettsia rickettsii)
- Babesiosis (Babesia)
If an infectious agent such as one of these is responsible for immune-mediated platelet destruction, obviously, specific therapy against the infection is warranted in addition to therapy for platelet destruction.
Very low platelet counts can also occur in response to the suppression of megakaryocytes within the bone marrow. This might be caused by:
Disseminated intravascular coagulation (DIC) is a life-threatening, disastrous failure of normal blood clotting and clot-dissolving functions in the body. One of its hallmark signs is a drop in platelet count, along with a constellation of other signs.
If platelet numbers are normal but it is obvious that platelet function is not, some other causes to look into might include:
Therapy for Immune-Mediated Platelet Destruction
Once a tentative diagnosis of immune-mediated platelet destruction has been made, the goal in therapy is to stop the antibody production. This, of course, means suppression of the immune system using whatever combination of medications seems to work best for the individual patient.
Prednisolone, Prednisone, or Dexamethasone
These steroid hormones are the first line of defense and, often, all that is necessary to bring platelet counts back up. Unfortunately, long-term use should be expected, and this means steroid side effects are eventually inevitable: excessive thirst, possible urinary tract infection, panting, poor hair coat, etc. The good news is that these effects should resolve once the medication is discontinued; further, if side effects are especially problematic, other medications can be brought in to reduce the dose of steroid needed. Prednisolone is the pre-activated form of prednisone.
Vincristine
This injectable medication is mildly immune suppressive but also stimulates a sudden burst of platelet release from the marrow megakaryocytes. The platelets released in response to vincristine contain a phagocyte toxin so that when they are ultimately eaten by spleen phagocytes, the phagocytes will die. While repeated injections of vincristine ultimately do not yield the same effect, at least a one-time dose may be extremely helpful. Vincristine is extremely irritating if delivered outside of the vein. It must be given by IV cleanly or the overlying tissue will slough. Vincristine is generally used for unstable or more severely affected patients.
Azathioprine, Cyclophosphamide, or Mycophenolate
When corticosteroids alone have not yielded a good response after a week or if a reduction in steroids dose is desired, a second immune-suppressive agent can be used. These medications may not have steroid side effects but they have other issues of their own that must be considered. Cyclosporine is an immune modulator often used in organ transplantation.

Photo courtesy of MarVista Vet
Transfusion
You might think that a transfusion of blood or at least platelet-rich plasma might be helpful in treating platelet dysfunction. The problem is that platelets do not survive well after removal from a blood donor. You have about 12 hours to deliver the freshly withdrawn blood to the recipient before the platelets become inactive. After the platelets are delivered, they are likely to live only for hours. In general, most efforts are spent on establishing immune suppression. That said, if the patient has had significant blood loss as a result of her platelet deficiency, a transfusion will certainly replace red blood cells, even if it cannot effectively replace platelets.
Gamma Globulin Transfusion
Gamma globulins are blood proteins, including antibodies. Human gamma globulin appears to occupy the spleen cell removal binding sites so that coated platelets cannot be grabbed out of the circulation.
This has been a promising therapy for both humans and dogs but is generally prohibitively expensive. Furthermore, research has shown that results are similar to those obtained simply by using vincristine. Since a less expensive treatment exists with less potential for side effects, gamma globulin therapy is rarely used.

Photo courtesy of MarVista Vet
Splenectomy
If the medication simply does not work or the condition keeps recurring once medications are discontinued, the solution may be to simply remove the spleen. After all, this is where the phagocytes removing the platelets are primarily located. In humans, immune-mediated platelet destruction is generally treated with splenectomy first. Response in dogs has not been as predictably good, thus in veterinary medicine, it is generally one of the last therapies invoked and is reserved for patients with recurrence issues.
TPO Receptor Agonists (Romiplostim and Eltrombopag)
Hepatic thrombopoietin is one of the factors the liver makes in response to removing old platelets from circulation. Remember, when platelet removal switches to the spleen in this disease, hepatic thrombopoietin is not generated, and the bone marrow may not be properly stimulated. These two agents have revolutionized ITP treatment in humans, so we bring them up here. They act by enhancing the marrow's response to hepatic thrombopoietin. The problem is that eltrombopag does not bind to canine receptors, and studies of romiplostim in dogs are sparse. That said, it may not be long before research progresses and TPO receptor agonists are included in therapy.
Prognosis
The good news is that 70-90% of dogs with ITP will recover. Factors that bode poorly include:
- tarry black stools (indicating bleeding in the small intestine.)
- an increase in the blood urea nitrogen test.
- illness severe enough to warrant blood transfusion. (These patients appear to have a higher relapse rate.)
Treatment continues long after the patient appears to have recovered, with the immune-suppressive agents tapered down slowly over several months. Recurrence occurs in approximately 30% of affected dogs and most commonly occurs after two to three months from diagnosis. When recurrence happens, medications must be stepped up. Of the dogs that suffer a recurrence, approximately 50% will suffer yet another one. Splenectomy results in permanent remission in approximately 60% of patients and is likely a good choice for a dog with a recurrence problem.