
Graphic by Marvistavet
(Also called sacrocaudal fractures in cats)
First, an Anatomy Lesson
Tails are wonderful, expressive body parts used by cats for communication purposes as well as for balance. The tail consists of a varying number of vertebrae (called caudal vertebrae; caudal means near or at the tail) and voluntary muscles with ligaments and tendons holding it all together. The tail attaches to the body at an area called the tail head. The first caudal vertebra attaches to a backbone called the sacrum, which connects the tail and lower back (lumbar) vertebrae.
The "Horse's Tail"
The spinal cord does not extend down to the tail (it typically ends at the level of the fifth lumbar vertebra), which means that tail injuries do not damage the spinal cord. Unfortunately, injuries to the tail can still cause serious nerve damage.
Spinal cord and caudal equine of a cat
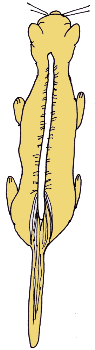
The spinal cord ends around the level of the 5th lumbar vertebra. The nerves coming off the spinal cord must stretch out behind in order to serve the body parts to the rear of that vertebra. This creates a pony tail of nerves called the caudal equine, which literally means "horse's tail." Graphic by MarVistavet
Cats get their tails pulled or broken through an assortment of traumas: A child might pull a tail or it might get caught in a closing door. A tail can get bitten during a cat fight and, of course, automobile accidents can easily lead to dislocated or broken tails. One might think a tail break would involve an obvious external wound but usually this is not the case; instead, signs of nerve damage from stretching of the cauda equina nerves are often the only tip off.
In many cases, the tail pull injury is eclipsed by bigger injuries. In one study presented at the World Small Animal Veterinary Association Congress in 2016, 46% of tail pull injuries were accompanied by pelvic fractures or sacroiliac dislocations, 18% were accompanied by broken rear legs, and 11% had additional spinal fractures. Only 21% had the tail pull as the only injury.
Because the spinal cord ends so high up, nerves exiting the cord to provide control and sensation to the tail, hind legs, urinary bladder, large intestine, and anus must extend long branches to reach their destinations. When you look down at these nerves (an aerial view if you will), these nerves are said to look like a horse’s tail, and thus anatomists call this area the cauda equina (which literally means horse's tail).
What Might be Noticeable at Home After a Tail Pull Injury
Cats with a tail pull injury might show any of these symptoms:
- A tail that drags or is never held high.
- Involuntary dribbling of urine.
- A dilated, flaccid anal sphincter with or without diarrhea or fecal incontinence.
- Incoordination of the rear legs.
Any of these symptoms might lead the cat into the vet’s office for an evaluation. Some additional findings the veterinarian might notice include:
- A distended bladder that is relatively easy to express manually (in other words, the bladder is full but can be emptied with careful squeezing.)
- Bloody urine (if the tail trauma is recent).
- Painful tail head.
- Loss of sensation in the tail.

The cat in this radiograph has a dislocation of the tail between the first and second caudal vertebrae (see flashing red arrows). Also note the distended urinary bladder (flashing yellow dotted line). Photo by MarVistaVet
A radiograph will often show a break in the tail or a dislocation, although in some cases the tail bones are intact. How permanent these signs are largely depends on whether the cauda equina nerves have been over-stretched or actually torn.
Classification of the Injury
In a 1985 study by Smeak and Olmstead, sacrocaudal fractures in cats were divided into five groups.
Group One: Cats With Painful Tail Heads as their Only Sign
These individuals are minimally affected and, while they may or may not have a chronically sensitive tail head, they are expected to otherwise have a full recovery.
Group Two: Cats With Lack of Tail Mobility and Sensation as Their Only Sign
These cats are expected to recover tail function completely and have an excellent prognosis.
Group Three: Cats With Lack of Tail Mobility and Sensation Plus Urine Retention as Their Only Signs
Most cats will have a complete recovery.
Group Four: Cats With Lack of Tail Mobility and Sensation and Diminished Anal Tone
This group of cats has about a 75% recovery rate, meaning 75% of the cats that fit this description should recover.
Group Five: Cats With Lack of Tail Mobility and Sensation Plus a Dilated/Flaccid Anus (i.e., Zero Anal Tone)
This group of cats has about a 50% recovery rate, meaning about half of the cats with this description will eventually recover.
If it is not clear whether a cat has partial anal sphincter tone or not, it may be possible to have a test called an electromyogram. The muscles of the anal sphincter and tail can be tested to see if they are receiving any nerve input at all. If they are, there is reasonable potential for recovery. The EMG test is highly specialized and not readily available except at practices with a neurology specialty. Referral will probably be necessary.
In a more recent study (Nov 2009, Journal of Small Animal Practice) researchers found that an excellent predictor of bladder function return is pain detection at the tail head. In the 21 cats with sacrocaudal fracture/dislocation, all 11 cats that had pain sensation at the tail head on the first day after the injury had regained bladder function within 3 days. Absence of pain sensation in this area on the first day did not necessarily mean that bladder control would not return; 60% of cats without tail head sensation on the first day had recovered bladder control by 30 days after the injury.
Should the Tail be Amputated?
If the tail is not expected to recover mobility or sensation, there are some reasons to consider amputation. If the cat cannot lift his tail, he may soil it regularly, creating an infection issue or simply an odor issue. Further, the weight of the tail dragging may further stretch the cauda equina nerves. Whether or not tail amputation is helpful or speeds recovery is controversial but certainly amputation could solve a soiling problem.
Bladder Management
It is important not to allow the bladder to over-stretch. The fine muscles of the bladder can become so stretched out that even if the nerves recover, the bladder may still remain unable to empty fully. This means the cat’s bladder must be gently squeezed three or four times daily to keep it from over-distending. Medications can also be used to assist the bladder’s own ability to contract (bethanechol chloride) or to relax the urinary sphincter (prazosin or phenoxybenzamine). Since urine retention tends to promote infection, patients will periodically require some sort of monitoring urine tests. If constipation is a problem, periodic enemas or stool softening medications can be given regularly.
Recovery Time
Nerves heal notoriously slowly. It has been said that a good six months must pass before one can say the maximum recovery has occurred and no more positive progress can be expected. Most cats who are going to recover function do so in a one-week period, and most cats who do not recover urinary control after a month probably will remain incontinent. Tail function and sensation tends to take longer.
Information for this article was largely drawn from:
Lanz, O.I., Lumbosacral and pelvic injuries. Veterinary Clinics of North America Small Animal 32 (2002) p 949-962.