ventral lesion
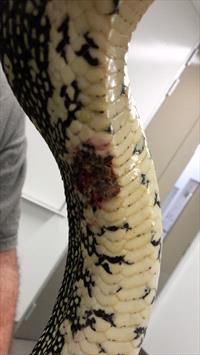
This Diamond python has a focal bacterial dermatitis lesion. Photo by Dr. Oliver Funnell
Bacterial dermatitis in reptiles is described as a superficial or deeper infection of the skin or shell with bacterial organisms. There are many names used for this disease that you may hear including septicemic cutaneous ulcerative disease (SCUD), shell rot, belly rot, and blister disease. The correct diagnosis is critical in these cases because bacterial, fungal, and burn lesions all look similar. It is important to work with your veterinarian to get the correct diagnosis. In the majority of cases of bacterial dermatitis in reptiles, consideration should be given to the presence of underlying disease and environmental stressors (inadequate husbandry) leading to immunosuppression and secondary bacterial infection leading to dermatitis.
Bacterial dermatitis is typically focal (one or two areas only) or localized but may be more extensive or generalized over a large portion of the body.
In the early stages of bacterial dermatitis, owners may see pustules and/or blisters. These will rupture and typically cause an open wound. These wounds may be shallow or may be deep enough to expose muscle or bone (this is more often seen in the shells of turtles). These lesions may be single or multiple, and if multiple lesions are present, they may join together to form larger wounds.
In many cases, bacterial dermatitis develops after a traumatic event that caused abrasions or lacerations that allowed the bacteria a path into the skin. The longer the delay in taking the affected reptile to the veterinarian, the worse the condition becomes and the more difficult to treat, as the reptile begins to have a poor body condition and becomes depressed and isn’t hungry. Lesions that have been present for a few weeks often become thickened or bumpy (hyperkeratotic).
Bacteria that cause dermatitis in reptiles are often Gram-negative and there is a wide variety of bacteria in this category that can lead to disease. Mixed infections involving more than one bacterium are not uncommon.
In general, for the vast majority of cases bacterial dermatitis is not contagious to humans. However, there are a few organisms that can be zoonotic to humans, and so a diagnosis is important in these cases.
As for the reptiles themselves, other animals kept in the same deficient captive environment may develop identical skin lesions.
Examples of bacterial dermatitis diseases include:
Blister Disease
This is commonly seen in snakes and is characterized by extensive dermatitis, often accompanied by the formation of blisters. Blister disease is a condition in which snakes develop multiple vesicular or bullous (blister-like) skin lesions normally seen on the belly of affected snakes. The most common cause for blister disease in snakes is poor husbandry conditions, such as excessive humidity (wet conditions), inadequate substrate, dirty conditions, incorrect temperatures, or any combination thereof.
Septicemic Cutaneous Ulcerative Disease (SCUD)
SCUD is an old and inaccurate term used for a more generalized form of bacterial dermatitis, often ulcerative, of the upper or more commonly the lower shell in aquatic turtles; it is seen most commonly as multiple ulcers and wounds over the shell. Pond turtles, softshell turtles, and snapping turtles are sometimes diagnosed with this disease. Poor water quality is typically the major reason for the disease, caused by inadequate filtration and/or insufficient water changes. This disease may lead to septicemia and death.
Devrieseasis
Devrieseasis is caused by the bacteria Devriesea agamarum and is a disease of mostly desert-dwelling and dry land lizard species such as Uromastyx sp, bearded dragons, collard lizards, and other Agama sp. and is often characterized by the presence of bumpy growths along the upper and lower lips, especially at the corners of the mouth. In some cases, the disease can lead to abscesses under the skin and septicemia.
Affected Reptiles
Reptiles of all species and ages, and of both sexes, are susceptible to bacterial dermatitis. Young and geriatric animals may be more susceptible because of immature or weakened immune systems. Although purely anecdotal, accounts suggest that color mutants or morphs may be more susceptible generally thought to be from reduced immune function in these color mutations. Bacterial dermatitis in captive reptiles occurs worldwide, and no seasonality has been documented. In temperate climates, animals have no access to sunshine in autumn/winter/spring and may be more susceptible.
Certain species of reptiles may be predisposed to trauma, which often leads to bacterial dermatitis. Green water dragons and basilisks are flighty lizards that often damage their faces. Some snakes rub their noses and faces against the enclosure walls to the point of damaging themselves; these abrasions may easily lead to infection. Iguanas, bearded dragons, and other long-tailed lizards often damage the end of the tail, which may lead to bacterial invasion and infection.
It is not too much of a stretch to say that deficient or substandard husbandry probably underlies all cases of bacterial dermatitis in reptiles.
ventrum 3
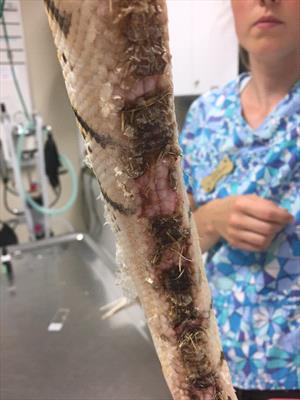
This ball python has a generalized bacterial dermatitis of the ventrum, which is commonly called blister disease. Photo by Dr. Sarah Barnes.
Diagnosis
In any suspected case of bacterial dermatitis, a diagnosis should be based on a multidirectional approach using different tests including cytology (examining types of cells on your pet's skin) and histopathology (examining tissue samples). In other words, just because bacteria are present does not mean they are causing disease. To diagnose bacterial dermatitis, your veterinarian will begin with a thorough husbandry history and physical examination and perform some diagnostic testing including a complete blood count and serum chemistry panel. In addition, he will likely want to take x-rays to assess the extent of the lesions and also collect some fluid from any blisters to analyze in the clinic to see if there are any bacteria. If there is, the fluid will be sent out to a laboratory to be cultured to determine the appropriate antibiotic to use. Bacterial dermatitis lesions can closely resemble lesions caused by fungal organisms; some viruses (such as the Pox virus); thermal burns; and some nutritional problems such as low vitamin A.
Your veterinarian will concentrate on a detailed history of husbandry, so be prepared to answer numerous questions about temperature, humidity, and hygiene. Lighting also affects reptile health. Your veterinarian will ask about any sharp objects or rough surfaces in the captive environment, and whether or not the reptile is rubbing anything, which may cause lacerations or puncture wounds.
In many cases, your veterinarian may suggest additional testing to arrive at the proper diagnosis. Some of the commonly performed tests include a blood culture that will reveal any causative bacteria in the blood. A biopsy is the preferred and most common test to get a definitive diagnosis. Biopsies that remove the lesion, called excisional biopsies, may also be curative. If lesions are too numerous, your veterinarian will collect several representative lesions for an analysis that will include histopathology (tissue testing) at an outside laboratory.
softshell turtle
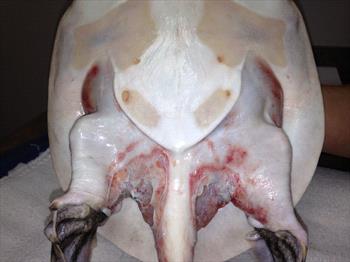
A soft-shell turtle with ulcerative bacterial dermatitis. Photo by Dr. Missy Jewell
Treatment
The initial and long-term treatments that your veterinarian will prescribe for a reptile with bacterial dermatitis will vary depending on the type of reptile, its current condition, and the extent of the disease. In all cases, correcting any husbandry deficits is critical or no treatments will be effective and the condition will reoccur. If the reptile is dehydrated, your veterinarian will provide fluids by soaking or by injection to rehydrate the patient and stabilize them.
Deep or extensive lesions may need to be surgically cleaned up and dead tissue removed (debridement) under anesthesia. Your veterinarian will determine the best antibiotic to use based on the culture or your veterinarian’s experience. In most cases, topical antibiotics will be prescribed (such as silver sulfadiazine [Silvadene]), and systemic (injected) antibiotics.
Except for large defects, infected skin typically heals better without a bandage. But in some cases, a wet-to-dry bandage that is changed daily is needed to help with healing.
It is common while treating water turtles to use a technique called dry-docking (keeping an aquatic turtle out of the water) for one to two hours daily, or longer as necessary; this allows topical treatment to be applied more efficiently, and the drying may help treat pathogenic bacteria.
It is important to give the treatments prescribed by your veterinarian exactly how and for the length of time they are prescribed. Treatments typically should not be discontinued before the patient is brought back to the clinic and the progress or resolution of lesions has been assessed by your veterinarian.
After debridement 1
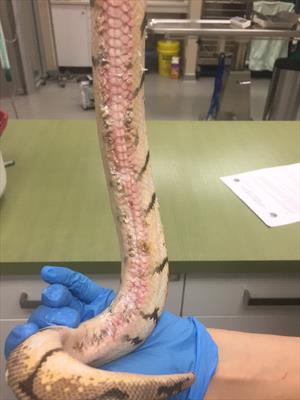
The same ball python as above after surgical debridement of the bacterial dermatitis lesions. Photo by Dr. Sarah Barnes.
Prognosis And Prevention
Prognosis will depend greatly on the severity and extent of lesions, the nature of any underlying disease, and the ability to pinpoint and correct husbandry deficiencies. Scarring is a common outcome of dermatitis and should not be confused with active lesions. These cutaneous scars in reptiles appear as unpigmented, whitish/grayish, smooth, sometimes with a black rim, contracted (shrunken, tighter), or wrinkled areas, where lesions previously existed.
Bacterial dermatitis in captive reptiles reflects husbandry inadequacies and/or underlying disease. As our understanding of the care of various captive reptile species increases, the incidence of bacterial dermatitis is likely to decrease.
Awareness by owners of proper husbandry requirements for the species in their care will minimize the risk for bacterial dermatitis.