The Cornerstone of Treatment
Assuring optimal hydration is the single most important aspect in the treatment of kidney disease. The kidneys are made up of millions of small filtration units called “nephrons.” Nephrons receive all the materials circulating in the bloodstream and must separate out the good stuff to keep (proteins, sugars, electrolytes etc.) from waste to be dumped (toxins, excess material etc.). The good stuff stays in the bloodstream while the waste is dissolved in water and made into urine. Because water is "good stuff" in and of itself, the kidney is designed to get rid of the waste material in the smallest amount of water possible.
Urine is made constantly and continuously by the kidneys. The ureters connect the kidney to the urinary bladder so that urine can be transported there and the bladder stores the urine until it is convenient to dump it into the environment. The system is very efficient and precise but it is driven by water. If the body becomes dehydrated, the kidney can't do its job.
Nephron
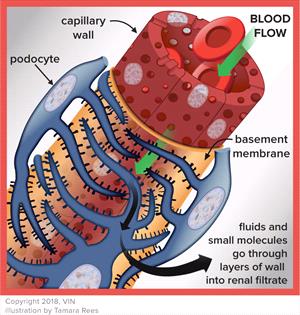
Drawing Courtesy Tamara Rees
Over a lifetime, nephrons are damaged and are no longer able to participate in the filtration process. They die from poor circulation, they become clogged by toxin sludge, or they may simply wear out. This is normal and is part of the wear and tear of living. Fortunately, we have many extra nephrons so losing some is not a big problem; that is, not a big problem until we have lost about two-thirds of them. At this point the remaining nephrons will have trouble keeping up with the waste removal demands of the body. Extra water is needed to remove the same amount of metabolic toxin so the patient begins to drink more. There may come a point where drinking water will not keep up with the toxin load and the patient will feel sick. Feeling sick means less activity and less water consumption which makes it even harder to get rid of the toxin load and a vicious cycle has been created.
This means that if the kidney disease is not detected until the patient is already feeling sick, less than one-third of the original number of nephrons are left. We need to maximize the efficiency of these remaining nephrons, and hopefully slow down their loss. We also need to get rid of enough toxin for the patient to feel good again.
The build-up of toxins is called "azotemia." Actually feeling sick from the toxins is called "uremia." Your pet can have azotemia without uremia but if they have uremia, they certainly also have azotemia.
Diuresis
Diuresis is the medical term for increased urine production. The patient may have already been doing this somewhat by drinking excessively but there comes a point when it is not possible to drink enough and toxins build up as mentioned. When the patient first begins to feel sick, he tends to eat less and drink less. Dehydration results, which is disastrous for the patient that already had an increased need for fluids to start with. To solve these problems, we will need to correct the dehydration and maximize the circulation through the remaining nephrons. This is accomplished by giving the patient more fluid, either intravenously in the hospital or under the skin in either the hospital or the home setting.
Intravenous (IV) Fluid Therapy
Dog on IV Fluids

Photo by MarVistaVet
Intravenous fluid therapy involves placing an intravenous catheter in the leg or neck so that a continuous drip of fluids can be given directly into the bloodstream. The procedure is not painful nor stressful as after the catheter is placed, the patient simply relaxes in a hospital cage. After two or three days, lab tests are repeated to see what parameters have changed. Therapy is revised at that point to either continue IV fluids or discharge the patient with a new plan for home treatment.
IV fluid therapy offers many benefits to the kidney patient:
- Continuous hydration means continuous maximized nephron activity and the most efficient toxin removal.
- Rapid response to treatment (days).
- Because hospitalization is needed for this treatment, a professional staff will be monitoring the patient's progress and can make rapid adjustments in adjunct therapy.
The disadvantages of IV fluid therapy include:
- Expense of hospitalization.
- Occasionally a patient dislikes the bandaging associated with the catheter and chews the catheter out. This incurs additional expense as the catheter is replaced and potentially the patient may need to wear an Elizabethan collar, which could be uncomfortable.
- Stress from separation of pet and owner, though we find in most cases that it is the owner's stress and not the pet's that dominates. Most animals are comfortable in their cages, nothing that generates fear is happening, and they quickly habituate to the cage environment and activity viewed through the bars.
Subcutaneous Fluids in a Cat

Photo by MarVistaVet
Subcutaneous Fluid Therapy
The word subcutaneous means under the skin. Here, fluids are given all at once in a pocket under the skin and the patient absorbs them gradually. Initially, intravenous fluid therapy is generally considered superior to subcutaneous fluid therapy but this depends on the blood test results of the patient; some are able to skip straight to subcutaneous fluids or are forced to by the expense of intravenous therapy. Fluids are typically given every couple of days with the frequency increasing if the pet gets worse or decreasing as the pet gets better.
Advantages of subcutaneous fluids include:
- The procedure is easy for a client to learn and perform at home. Separation from the pet is not needed.
- Because hospitalization is not needed, this form of therapy is much less expensive.
- The procedure can be performed in the hospital on an outpatient basis if the patient is not cooperative at home.
- Therapy is performed usually only every couple of days (though in more advanced cases could be once or even twice a day).
Disadvantages of subcutaneous fluids include:
- The owner must be comfortable with sticking a needle into the pet's skin. This psychological hurdle is generally overcome after the owner performs the procedure a couple of times. There are also implantable injection ports available.
- Changes in toxin level tend to occur more slowly (weeks). This makes subcutaneous fluids less appropriate for more advanced cases.
- Large dogs often require inconveniently large volumes of fluids.
- Some patients attempt to hide from the owner when they think the needle is coming and some people feel this changes the relationship with their pet in a negative way that may not justify the health benefits. It is important to realize that this is not the usual experience with subcutaneous fluids; most people find that the comfortable life quality for the rest of the day or next several days more than compensates for the 10 minutes of unpleasant fluid administration. Most pets are cooperative for fluid administration.
See more details on how to give subcutaneous fluids.
An alternative form of fluid administration utilizes the patient's own GI tract via an esophagostomy tube. The tube allows for relatively large amounts of water to be given without needles or hospitalization. In patients where heart disease is concurrent with kidney disease, there is a delicate balance that must be met between making the kidneys happy with extra circulating fluid yet not creating a fluid overload on the compromised heart. The GI tract creates a buffer in this situation; extra fluids will simply not be absorbed into the body. The esophagostomy method may lead to a loose stool but is much safer for a weak heart. Using the esophagostomy tube to give fluids also prevents you from struggling with a syringe into the pet's mouth. Such struggling is unpleasant for all parties involved and can lead to fluid aspiration into the lung. Use of the esophagostomy tube is generally struggle-free and by-passes the respiratory tract.
The esophagostomy tube is placed through a small hole in the esophagus (the passage connecting the mouth and stomach). Fluids can be administered through this tube and into the stomach thus avoiding the needle stick. The tube can stay comfortably in place for months but the hole will require regular cleaning and bandaging at home. A pet with an Esophagostomy tube should not be allowed outside unattended in case the tube or wraps become entangled in bushes, fences etc. General anesthesia is required for placement of this tube.
In Conclusion
The importance of hydration cannot be overemphasized in the treatment of kidney disease and the degree of uremia will dictate how aggressive treatment will need to be. Most patients will require a maintenance fluid therapy plan of some kind to make sure they are hydrated regularly. Your veterinarian will be able to guide you to the best fluid plan for you and your pet.